The field of nursing is one of the most respected in the world. Nurses are the links between doctors and their patients. They are the humanity behind the diagnosis, the pillar of women going into labor, and the backbone of patient care in every hospital, and clinic.
Want to Stop Leg Swelling Now?
ComproGear Compression Socks are designed to stop swelling instantly!
Click the button below to see the lineup of ComproGear Compression Socks:
Nursing is a rewarding career with many benefits. According to the Bureau of Labor Statistics, there will be a major shortage of nurses. The population is growing much bigger each day and so medical facilities are always looking for more nurses. Some facilities even add $10,000 bonuses for signing on. Pursuing a career in nursing could be rewarding in the long run.
It is also a very exciting career. Unlike a lot of professions, nurses see something different every day. The profession presents a new challenge, point of view, and people with each day. Some people in the profession have described it as a daily adrenaline rush.

Becoming a nurse gives you the flexibility to work almost anywhere. You will find that there are many nursing jobs available almost everywhere you go.
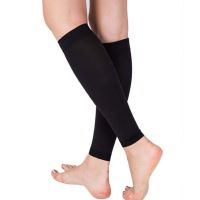

What is more, you can work in clinics, hospitals, private practices, and rural areas. If you become a freelance consulting nurse, then you can travel to all parts of the country; moving from place to place as you like.
Nursing offers more than 200 specialties where you can earn an official certificate. Specialties make you more knowledgeable and experienced in your field. This will certify that you are an expert in a certain specialty making you more desirable to medical facilities. It will also boost your salary.

If you already have a career, then nursing can be a great second career for you. It is one of the most popular second career choices in the world. Many professionals retire after their first careers then pursue nursing as a second career. The work would be just as if not more fulfilling than your first career. You can get an education online and in almost every location in the world.

Even better, when you do graduate from nursing school, you will join the workforce faster than most professions. You can earn an associate degree or diploma in two to three years then join the workforce. There are also accelerated bachelor programs that allow you to complete your degree as fast as two years.

Above all, nursing is an exciting, and engaging career. Nurses everywhere make a real difference by saving lives every day; literally. They go above and beyond to care for maintenance. Even more than that, the majority of nurses volunteer in their communities with the aim of promoting public health and hygiene. Nursing is an ever-learning process as every challenge presents an opportunity to learn.

Unfortunately, there are a few things that nurses have to endure due to their career demands. The job requires you to be on your feet from most of the day helping patients, running tests, and so much more. This takes a toll on your body and nurses are not immune to this. Nurses face several medical problems with their legs due to the number of hours they are on their feet.

One such disease is varicose veins. Varicose veins are bulging, twisted, enlarged, and bluish veins that occur in the legs and feet. They look like bruised cords running down your legs; just beneath the surface of your skin.
They are visible and are sometimes surrounded by bluish visible capillaries that are known as spider veins. Spider veins sometimes occur as a mild form of varicose veins.
Causes of Varicose Veins
The blood vessels known as arteries in your body are responsible for transporting oxygenated blood from the lungs to the rest of the body. The arteries are surrounded by thick layers of muscle and tissue to help with this process.
The veins, on the other hand, are responsible for taking deoxygenated blood back to the lungs for oxygenation. Unlike arteries, veins do not have layers of muscle or tissue. They instead rely on surrounding muscles and a network of valves. As blood flows through the veins, the cup-like valves open to allow blood to flow through, then close to prevent backflow.

In varicose veins, these valves do not function properly. It could be because the walls of the veins have weakened, altering the function of the valves. Thus, blood will not flow back to the heart and instead pool at the feet and legs. Instead of moving from valve to valve, the blood pools in the vein which in turn increases pressure and congestion. This causes the veins to bulge and twist; and because superficial veins have less muscle support than deep veins, they are more likely to become varicose.
Want to Stop Leg Swelling Now?
ComproGear Compression Socks are designed to stop swelling instantly!
Click the button below to see the lineup of ComproGear Compression Socks:
Popular Articles on ComproGear
Wide Calf Compression Socks Your Guide To Compression Socks for Heavy Legs
Compression Stockings mmHg Chart What Does Mmhg Mean in Compression Socks?
Compression Sock Sizes How To Measure for Compression Stockings?
Plus Size Compression Socks ComproGear 5XL and 6XL Compression Socks Now Available
The most prevalent symptom of varicose veins is veins that are dark purple or blue in color. They are visible, bulging, and twisted. Your legs will feel achy, or heavy; the pain may worsen when you sit or stand for a long time. You may notice burning and itching in the affected areas as well. This is often followed by skin discoloration and spider veins around the affected area.
Risk Factors of Varicose Veins
Some situations or conditions put you at risk of developing varicose veins. one of the most common is age. Aging causes wearing, and tearing on your valves. The wear prevents the valves from closing properly which allows most of the blood to flow back into your veins where it collects instead of flowing up to your heart. Older nurses are more likely to develop varicose veins as they are also always on their feet.
Unfortunately, women are more likely to develop varicose veins than men due to hormonal changes that occur during pregnancy, menopause, and menstruation. The hormones released during these times tend to relax vein walls. Female nurses are more likely to develop varicose veins than male nurses.
Pregnancy is another risk factor for developing varicose veins. During pregnancy, your body retains fluids to increase the volume of blood in the body. This change is in order to support the growing fetus. Unfortunately, it produces enlarged veins in your legs.

Finally, standing for long periods of time greatly increases the chances of developing varicose veins. Nurses often develop varicose veins because they are always on their feet. This combined with other risk factors such as gender, and age almost always means that a nurse will develop varicose veins.
Varicose veins; if not treated brings about a number of complications such as blood clots. The legs affected by varicose veins become painful and swollen. If this goes on for a while, it becomes an indication that a blood clot formed within the vein. This condition is known as thrombophlebitis. Prolonged swelling and twisting of varicose veins sometimes cause a burst in the skin which leads to bleeding that requires medical attention.

For nurses, there is a lot you can do to prevent varicose veins. You can watch your weight, exercise regularly, eating less salt, increasing your fiber intake, and wearing flat comfortable shoes. However, these may not always work, and that is where compression wear comes in. Studies have shown that compression wear reduces aches and pain associated with varicose veins.
Want to Stop Leg Swelling Now?
ComproGear Compression Socks are designed to stop swelling instantly!
Click the button below to see the lineup of ComproGear Compression Socks:
However, they have not been proven to cure varicose veins. Still, they are very beneficial to nurses. Compression stockings put firm pressure on the legs and the varicose veins. This pressure helps to promote the circulation of blood. It prevents the pooling of blood in the varicose veins.

Another disease that nurses may develop because of standing for long periods of time is leg ulcers. A leg ulcer is a break in the skin of the leg. This break allows air and bacteria to enter into the underlying tissue. This condition is often caused by poor blood circulation.

Venous leg ulcers are the main type of leg ulcers that nurses develop. It occurs when the veins in your legs do not push blood back to the heart as they do. The pressure in the veins damages the skin which can break allowing bacteria in and causing ulcers.

Early signs and symptoms of leg ulcers include swelling of the legs and feet; which is often accompanied by pain. The skin in the affected area is dark red, or purple in color, and often turns hard. This is a sign of pooling. You will also feel itching and tingling in the affected areas.

When the ulcer develops, you will notice a shallow sore with a red base, and it is sometimes covered by yellow tissue. The borders of your legs and feet may look unevenly shaped. The surrounding skin will look shiny, stretched, and tight. It may also be warm or hot to the touch. Venous leg ulcers come with unbearable pain, especially when you stand for a long time. If the sore becomes infected, pus will drain fro it causing a bad smell.
Risk Factors of Leg Ulcers

As you would expect, people who develop varicose veins are at risk of developing leg ulcers. The two are almost always intertwined. People who develop varicose veins have tight stretched skin that can easily break with an injury. When it breaks, it provides the basis for developing leg ulcers.

People who have a history of Deep Vein Thrombosis are also at risk of developing leg ulcers. Deep vein thrombosis is when you develop blood clots deep in the veins. People who have developed blood clots before are at risk of developing leg ulcers.
Lymphatic obstruction can also put you at risk of developing ulcers in the legs. Lymphatic obstruction is the blockage of lymph vessels that drain fluid from tissues throughout the body. They also allow the immune cells to travel to parts of the body where they are needed.

Other uncontrollable factors such as being tall, being a woman, and aging can put you at risk of developing leg ulcers. Pregnancy also puts you at risk of leg ulcers for the obvious reason that you retain more fluids to increase blood volume in order to support the fetus. People who also stand for long periods of time such as nurses are also at risk of developing leg ulcers.
Why Should Nurses Wear Compression Socks?
Nurses work shifts of up to 12 hours; during this time, they are on their feet working and helping patients. As discussed, this will affect your leg health. Compression wear is the perfect addition to a nurse’s uniform.

When you wear compression socks, you will immediately notice that the pain and aching in your legs and feet will fade. Compression stockings improve blood circulation which makes it easier to deliver oxygenated blood to parts of the body. The oxygen stimulates muscles. Better circulation removes Lactic acid from your muscles which keeps your leg muscles strong even when you stand for long.

When you are done with your 12-hour shift, it is always advisable to wear your compression socks at home; before you go to sleep. This is because compression socks help with muscle recovery. They boost circulation which helps with muscle recovery when you are not working on your feet.
Want to Stop Leg Swelling Now?
ComproGear Compression Socks are designed to stop swelling instantly!
Click the button below to see the lineup of ComproGear Compression Socks:

One of the biggest reasons why nurses should wear compression stockings is that they get rid of discomfort. Nobody likes to be uncomfortable; especially at work. A nurse’s job is very critical and requires attention at all times. If a nurse’s attention is on the discomfort they feel in their legs and feet, then they will not be able to work well. Compression stockings greatly reduce discomfort brought about by these conditions.
Compression socks go beyond their function of improving blood circulation thanks to how they are made in terms of fabric. They do not roll down your legs and are aerated to prevent heat buildup. Some even have anti-microbial agents that prevent your feet from stinking.
Compression Stockings for Nurses

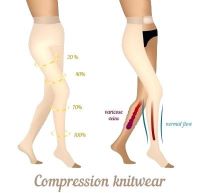
Compression stockings feature graduated compression. This type of compression means that the pressure applied by the stockings is greatest at the bottom of the legs around the ankle, the pressure then slowly decreases going up. Compression is measured in millimeters of mercury or mmHg. The larger the number, then the higher the compression levels.

There are different levels of compression available for nurses depending on their needs. Different compression levels serve different purposes; they are often prescribed by doctors. The most common is the 8-15 mmHg compression stockings. They offer the lightest form of compression and are great for energizing your legs. They provide relief from tired achy legs. This level of compression stockings helps to relieve mild swelling in the feet and ankles.

The second compression level is 15-20 mmHg. This is a mild compression level that provides relief from mild swelling, and pain. They provide relief from varicose vein related symptoms; especially during pregnancy. It is also this level of compression that prevents Deep Vein Thrombosis in nurses.

The next level of compression is the 20-30 mmHg stockings. This level of compression stocking is the most frequently prescribed level of compression. This level of compression greatly helps with the management of symptoms associated with varicose veins.
These compression stockings also help prevent the reappearance of varicose veins after surgical treatment. You can relieve symptoms of superficial thrombophlebitis wit this type of stockings. If you have a problem with the sudden fall in blood pressure or orthostatic hypotension, then you can benefit from these stockings.

The 30-40 mmHg compression stockings are a relatively high level of compression. They offer extra firm compression which is good for nurses who are working 12-hour shifts or more. These are great because they help manage symptoms of severe varicose veins. If your varicose veins have become severe with spider veins forming around them and major discoloration, then these stockings are for you.

This level of compression is best for the management of venous leg ulcers, Post Thrombotic Syndrome, Orthostatic Hypotension, and Postural Hypotension. Finally, it prevents the development of deep vein thrombosis.

The last level of compression available for nurses is 40-50 mmHg. This is a very high level of compression that is used in treating serious diseases. It is good for Acute Leg or Ankle swelling, Varicose veins, Deep Vein Thrombosis, and Chronic Vein Insufficiency. This level of compression is also known as Class III and it is often recommended by a doctor.
It is important to note that each level of pressure should be signed off by your doctor. Check with your doctor to determine what pressure level is good for you. Ensure that your doctor understands your routine well so that they can prescribe the right amount of pressure for you. Whichever level you choose, ensure that a professional measures you to ensure you are wearing the right size. The wrong size of compression stockings will do more harm than good.

Compression Stockings Buy Guide
No matter how strict your uniform should be, there is no need to go for a boring pair of compression stockings. Compression stockings come in a variety of colors and styles; there is something for everyone. Nurses especially are known for wearing colorful and brightly patterned compression socks. When you are buying, explore different colors, patterns, and themes. You can find all sorts of stockings in the market today. What is more, there are toeless, and footless options if that is whats you would like.
When buying compression stockings, ensure that you get the right size for you. Itis best to get a measurement done by a professional to determine your size. If your stockings are impossible to wear, or cutting off circulation to your legs, then they are too small for you.
If they are bunching up, not lying flat on your skin then they are too long for you. Often this will cause more discomfort. And, if they are a little loose, and keep sliding down, then they are too big for you or have lost their elasticity.
Fabric is the last thing you need to address. The evolution of compression wear has brought many fabrics into the game including spandex, cotton, nylon, lycra, and so many more. These fabrics will obviously feel different for you so the most important thing is that you find what feels best for you. Find the most comfortable fabrics for you and purchase compression socks. This ensures that your socks will not cause you more discomfort.
Want to Stop Leg Swelling Now?
ComproGear Compression Socks are designed to stop swelling instantly!
Click the button below to see the lineup of ComproGear Compression Socks:
