
Any profession can be demanding and exhausting. When working as a nurse, the stress of the job can especially take a toll on one’s health if proper rest and care isn’t taken. Using compression socks can help maintain good physical health. Doctors recommend knee pads and compression stockings for patients with edema, workers, travelers, professional athletes, and even nurses.
This article will explain how compression socks can be beneficial to nurses and how to choose the right pair.
The Nursing Profession

Nursing is one of the most admirable and timeless careers in history. Nursing dates back to the 19th century and was recognized worldwide by the efforts of Florence Nightingale during the Crimean War. Throughout history, nurses have treated men, women, children, and babies.
Nurses play a vital role in the healthcare field, as they focus primarily on patient care. They work in a variety of domains to improve public health and prevent and cure diseases and injuries. This is a profession that requires intense critical reasoning, judgment, communication, and evaluation skills. Nurses are not limited to war hospitals, but they are an essential contributor in all clinics, hospitals, and medical facilities. The current nursing profession adds some additional duties and responsibilities to nurses, including intensive care, medication management, food compliance, monitoring progress of recovery, and, in some cases, certified nurses may even prescribe medication.
Key Responsibilities
- Performing physical examinations and checking a patient’s medical history;
- Promoting the importance of health by providing counseling and education;
- Managing medications;
- Coordinating with various health care professionals.
Difficulties Faced
Nursing includes the combined care of patients of different ages, different backgrounds, and different nationalities and various physical and mental illnesses. Nurses need to assess their patient’s requirements based on their field; for example, nurses who work in cancer hospitals and nurses who work in burn treatment centers have different work fields.
Similarly, nurses work in emergency rooms, trauma centers, skincare centers, imaging centers, laboratories, clinics, and other medical centers. However, in almost all areas, nurses face many mental, physical, and emotional challenges. These difficulties or challenges include:
1. Occupational Hazards
Nurses come in contact with bacteria, harmful pathogens, and other dangerous liquids and materials daily, of which some have a direct impact on their health. Nurses also handle needles, sharp tools, and contaminated surgical equipment.
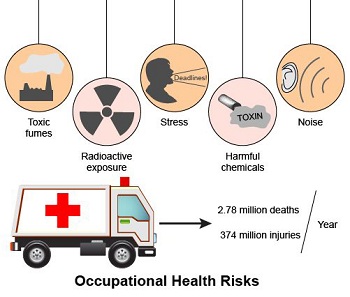
2. Tiredness and Exhaustion
Prolonged standing, sitting, and continuous movement can make a nurse feel tired and exhausted. Their legs and feet could even swell or ache, and they can face fatigue beyond just physical, but mental too.
3. Varied Working Hours
Work shifts vary, from 12 to 24 hours. These prolonged shifts can have severe short-term and long-term effects on the body, such as stress, fatigue, disturbed sleep cycles, and reduced social time with family and friends.

4. Limited or Shortage of Staff
Limited or shortage of nurses in hospitals and medical facilities causes an increase in the workload of existing staff and lead to longer working hours.
Causes of Swelling in Legs and Feet
In the medical profession, especially during emergencies, nurses must work quickly. Due to numerous duties and fast-paced activities which can lead to continuous work with barely any rest, the blood circulation can be affected, causing accumulation of blood or other fluids in the lower extremities.
If blood does not flow properly, this may cause discomfort and aches in the legs, as well as swelling in the feet or ankles. The risk is greater for nurses who frequently stand and walk.
Nurses may be required to supervise patients who are bedridden or need continuous medical attention. Long shifts can be exhausting and make nurses prone to edema in the lower and upper extremities.
Edema often occurs in people with reduced mobility. It may also be related to other conditions such as blood pressure, heart disease, diabetes, liver cirrhosis, and kidney disease.
However, persistent swelling in the feet or ankles may be a sign of a serious health problem. Should this occur, it is recommended that you consult with a medical health professional for advice and immediate treatment.
Prevention of and Treatment for Swelling in the Feet, Ankles, and Legs

1. Daily Exercise

Aerobic exercise, walking and stretching, can keep your body healthy and fit. Exercise can also help patients with edema by improving blood flow in the muscles and blood vessels of the extremities.
Nurses need physical exercise to keep them healthy and ensure proper blood circulation; an exercise routine could be adjusted according to work shifts and take short, in-between breaks to stretch the muscles.
2. Essential Oils
Cypress essential oil is, for example, a decongestant for the venous system, whereas peppermint oil is invigorating and refreshing, and cedar oil contains draining properties. Mixing five to seven drops of each oil then applying to the legs can help improve circulation and relief aches.
3. Cold Showers

The cold water can tone down dilated vessels and stimulate blood circulation.
4. Elevating the Lower Body During Rest
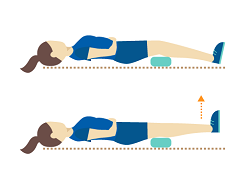
Lifting the lower part of the body is a temporary way to reduce swelling in the feet as it drains the fluid that has gathered there. Blood gradually leaves the lower extremities under the influence of gravity, and pain and soreness are somewhat relieved. Nurses and other health professionals can do this during breaks or at the end of the shift to reduce and prevent swelling.
5. Wearing Compression Socks
This is the main topic of this article, so continue reading to learn more!
What are Compression Socks?
Compression socks are hosiery designed to improve blood flow in the feet and legs.
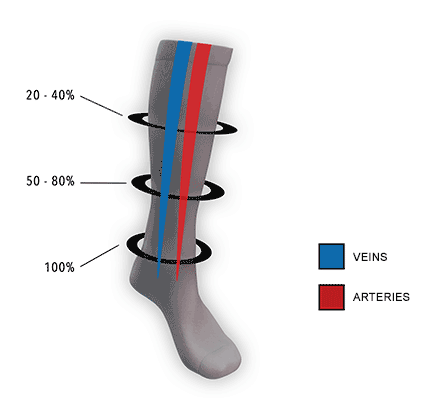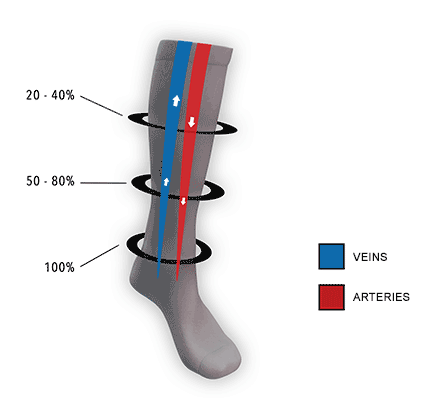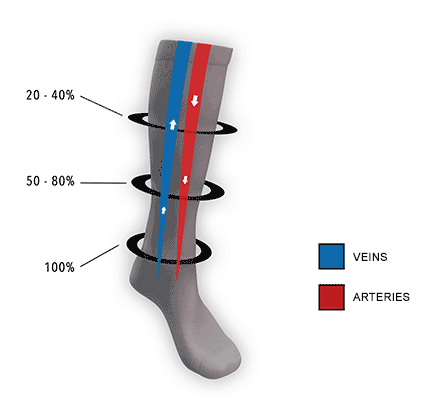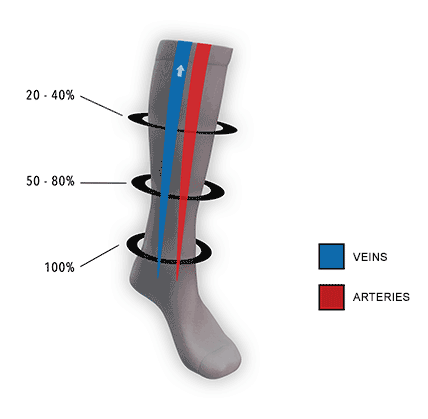
How They Work

Compression socks help increase blood flow and oxygen circulation and eliminate lactic acid from building up in the muscles.
Compression socks put pressure on your legs, feet, and ankles, which can:
- Increase the velocity of blood flow by reducing the diameter of the central vein,
- Helps prevent blood clotting.
Benefits of Compression Socks

Compression socks with a compression level of 20-30mmHg are perfect for nurses, as well as athletes, runners, doctors, pregnant women, and travelers, as they help rid aches quicker, whilst protecting calves, ankles, and feet.
1. Improve Blood Circulation and Reduces Micro-tears in Tissues and Muscles
By improving blood circulation, compression socks do not only help reduce cramps, tiredness, and swelling but also help in muscle recovery and reduce the risk of muscle and tissue damage that can occur from working long working hours.
2. Prevents Varicose Veins, Fatigue, and Coagulation
Compression socks can minimize leg fatigue, prevent foot and ankle pain, as well as prevent circulatory issues such as deep vein thrombosis (DVT), varicose veins, lymphatic disease, and blood clotting.
3. Helps Treat Other Circulatory Issues
They are very effective in treating and reducing edema, phlebitis, thrombosis, coagulation disorders and improving lymphatic detoxification. Doctors recommend knee-length socks and sleeves for patients with mild inflammation and chronic edema.
Types of Compression Socks
There are three types of compression socks:
- Graduated compression stockings,
- Anti-embolism socks, and
- Non-medical support hosiery.
Choosing the Right Pair

1. Material Composition

The materials used in compression socks are essential to nurses. Due to their profession, in which compression socks may be used for long hours, causing bacteria and sweat build-up, these socks would requires more cleaning.
Most materials used for socks are polyester, nylon, spandex, and fleece. Whether they are made from lightweight nylon or spandex material, compression socks can be extremely durable to provide support, comfort, and relief while working hard to care for patients. The reinforced/padded heel and toe support of the compression socks reduce muscle fatigue and offer maximum comfort, especially for walking for hours.
Ensure that you are not allergic to the material used in a pair of compression socks before purchasing.
2. Length and Compression Level
Male nurses tend to prefer knee-high compression socks, while women opt for thigh-high stockings. Nurses may require a mild compression level of either 8-15 mmHg or 15-20 mmHg.

Progressive compression is better for nurses and can improve blood flow to the feet and prevent swelling of the feet and ankles.
The optimal compression level for daily use is swelling of 15-20 mm Hg (mild or moderate compression), and for swelling of the feet, 20-30 mmHg (strongly compressed).
Just make sure to get the right size compression socks. There are now socks ranging from Small to 2XL, 3XL, 4XL, 5XL, and 6XL. In the past it has been hard to find even extra large compression socks. Now there are many more sizes than ever. So even if you need super plus size compression stockings that size is available.
Tips for Putting on and Maintaining Compression Socks
For maximum results, compression socks must be put on in the morning.
Below are some essential tips to make them easy to put on:

- Insert the hand inside the bottom and grab the heel,
- Flip the bottom upside down to the heel,
- Insert the foot and put the foot down to the heel without pulling,
- Climb down to the ankle, knee or thigh (depending on the length),
- Shoot the tip to release the toes.
Various accessories are available in the market to help you put them on.
The maintenance of compression socks differs from non-compression socks.
It is best that they are not washed in a washing machine nor put in a dryer. They must be washed by hand, in lukewarm or cold water, with a mild soap, then air dried. Avoid using bleach.
You should replace compression socks every six months if you wear them daily.
Conclusion
Nurses can have more physical support when carrying out their work by wearing compression socks throughout their shift. Not only are they able to be more productive with better leg and feet health, they are at a reduced risk of developing circulatory issues in their lower extremities.
This page last updated October 24, 2022
